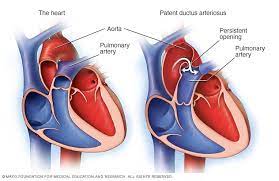
Patent Ductus Arteriosus is an extra blood vessel found in babies before birth and just after birth.In most babies who have an otherwise normal heart the PDA will shrink and close on its own in the first few days of life. If it stays open longer, it may cause extra blood to flow to the lungs. Problems are most likely if the PDA is large. Some smaller PDAs that don’t close early will seal up on their own by the time the child is a year old.
A patent ductus arteriosus is more likely to stay open in a premature infant, particularly if the baby has lung disease. When this happens, doctors might need to close the PDA.
Patent Ductus Arteriosus : What Happens in Patent Ductus Arteriosus?
The ductus arteriosus is a normal blood vessel that connects two major arteries — the aorta and the pulmonary artery — that carry blood away from the heart.
The lungs are not used while a foetus is in the womb because the baby gets oxygen directly from the mother’s placenta. The ductus arteriosus carries blood away from the lungs and sends it directly to the body. When a new-born breathes and begins to use the lungs, the ductus is no longer needed and usually closes by itself during the first 2 days after birth.
If the ductus doesn’t close, the result is a patent (meaning “open”) ductus arteriosus. The PDA lets oxygen-rich blood (blood high in oxygen) from the aorta mix with oxygen-poor blood (blood low in oxygen) in the pulmonary artery. As a result, too much blood flows into the lungs, which puts a strain on the heart and increases blood pressure in the pulmonary arteries.
In infants born with other heart problems that decrease blood flow from the heart to the lungs or decrease the flow of oxygen-rich blood to the body, the PDA may actually help, and the doctor might prescribe medicine to keep the ductus arteriosus open.
What Causes Patent Ductus Arteriosus?
The cause of PDA is not known, but genetics might play a role. PDA is more common in premature babies and affects twice as many girls as boys. It’s also common among babies with neonatal respiratory distress syndrome, babies with genetic disorders (such as Downs Syndrome), and babies whose mothers had rubella (also called German measles) during pregnancy.
What Are the Signs & Symptoms of Patent Ductus Arteriosus?
Babies with a large PDA might have symptoms such as:
- A bounding (strong and forceful) pulse.
- Fast breathing
- Not feeding well
- Shortness of breath
- Sweating while feeding
- Tiring very easily
- Poor growth
How Is Patent Ductus Arteriosus Diagnosed?
If a PDA is suspected, the doctor will use a stethoscope to listen for a heart murmur, which is often heard in babies with PDAs. Follow-up tests might include:
- A Chest X Ray.
- An ECG, a test that measures the heart’s electrical activity and can show if the heart is enlarged.
- An echocardiogram, a test that uses sound waves to diagnose heart problems. These waves bounce off parts of the heart, creating a picture of the heart. In babies with PDA, an echo shows how big the opening is and how well the heart is handling it.
- Blood tests
How Is Patent Ductus Arteriosus Treated?
The three treatment options for PDA are medicine, catheter procedures, and surgery. A doctor will close a PDA if the size of the opening is big enough that the lungs could become overloaded with blood, a condition that can lead to an enlarged heart.
A doctor also might close a PDA to reduce the risk of developing a heart infection known as endocarditis, which affects the tissue lining the heart and blood vessels. Endocarditis is serious and requires treatment with intravenous (IV) antibiotics.
- Complex paediatric heart defects:
Atrioventricular canal (AVC or AV canal Defect).
AVC is a heart problem that involves several abnormalities of structures inside the heart. These include atrial septal defect, ventricular septal defect, and improperly formed mitral and/or tricuspid valves.
Some of the problems that cause too little blood to pass through the lungs include the following:
- Tricuspid atresia.
- In this condition, the tricuspid valve does not form. Therefore, no blood flows from the right atrium to the right ventricle. Tricuspid atresia is characterized by the following:
- A small right ventricle
- Poor blood flow to the lungs
- A bluish colour of the skin and mucous membranes caused from a lack of oxygen (cyanosis).
A series of surgical procedures are often needed to increase the blood flow to the lungs and establish separate circulations.
Pulmonary atresia.
- A congenital defect in which the pulmonary valve or artery are underdeveloped. Normally, the pulmonary valve is found between the right ventricle and the pulmonary artery. It has 3 leaflets that function like a one-way door, allowing blood to flow forward into the pulmonary artery, but not backward into the right ventricle. With pulmonary atresia, problems with valve development prevent the leaflets from opening, therefore, blood cannot flow forward from the right ventricle to the lungs.
Transposition of the great arteries.
- With this congenital heart defect, the positions of the pulmonary artery and the aorta are reversed, thus:
- The aorta originates from the right ventricle, so most of the oxygen-poor blood returning to the heart from the body is pumped back out without first going to the lungs.
- The pulmonary artery originates from the left ventricle, so that most of the oxygen-rich blood returning from the lungs goes back to the lungs again
-
Tetralogy of Fallot.
This condition is characterized by the following 4 defects:
-
- An abnormal opening, or ventricular septal defect, that allows blood to pass from the right ventricle to the left ventricle without going through the lungs
- A narrowing (stenosis) at, or just beneath, the pulmonary valve that partially blocks the flow of blood from the right side of the heart to the lungs
- Thickening or enlargement of the right ventricle
- An “overriding” aorta (the aorta lies directly over the ventricular septal defect)
Tetralogy of Fallot can cause bluish colour of the skin and mucous membranes due to lack of oxygen (cyanosis).
Double outlet right ventricle (DORV).
A complex form of congenital heart defect, in which both the aorta and the pulmonary artery are connected to the right ventricle.
Truncus arteriosus.
During normal foetal development, the aorta and pulmonary artery start as a single blood vessel, and then the vessel divides into 2 separate arteries. Truncus arteriosus occurs when the single great vessel fails to separate completely. This leaves a large connection between the aorta and the pulmonary artery.
Some of the problems that cause too little blood to travel to the body include the following:
Coarctation of the aorta (CoA).
- In this condition, the aorta is narrowed or constricted. This obstructs blood flow to the lower part of the body and increases blood pressure above the constriction. Usually there are no symptoms at birth, but they can develop as early as the first week of life. If severe symptoms of high blood pressure and congestive heart failure develop, surgery may be considered.for more information
Congenital Aortic stenosis (AS).
- In AS, the aortic valve between the left ventricle and the aorta did not form properly and is narrowed. This makes it difficult for the heart to pump blood to the body. A normal valve has 3 leaflets or cusps, but a stenotic valve may have only 1 cusp (unicuspidal) or 2 cusps (bicuspid).
Although aortic stenosis may not cause symptoms, it may worsen over time. Surgery or a catheterization procedure may be needed to correct the blockage, or the valve may need to be replaced with an artificial one.
A complex combination of heart defects known as hypoplastic left heart syndrome can also occur :
Hypoplastic left heart syndrome (HLHS).
- A combination of several abnormalities of the heart and the great blood vessels. In HLHS, most of the structures on the left side of the heart (including the left ventricle, mitral valve, aorta, and aortic valve) are small and underdeveloped. The degree of underdevelopment differs from child to child. The left ventricle may not be able to pump enough blood to the body. HLHS is fatal without treatment.